Core Concepts of US Healthcare
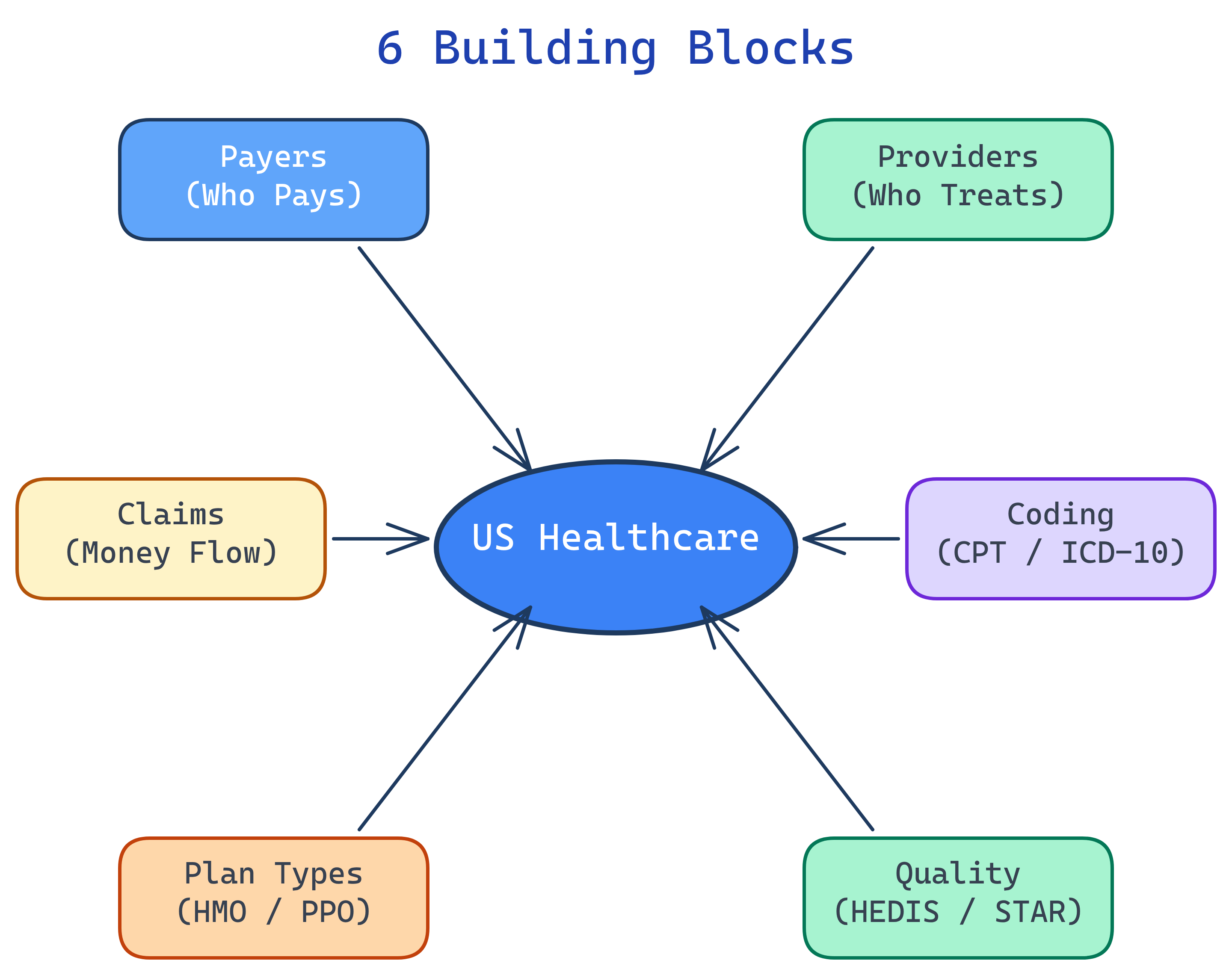
US Healthcare has 6 building blocks: Payers (who pays), Providers (who treats), the Claims Lifecycle (how money flows), Coding Systems (CPT/ICD-10), Plan Types (HMO/PPO), and Quality Measures (HEDIS/STAR).
The Big Picture
Every dollar in healthcare touches these six building blocks. Understand them and you understand the system.
Explain Like I'm 12
Think of healthcare like ordering food delivery. The restaurant is the provider (doctor). The delivery app is the payer (insurance). The menu uses special codes (CPT/ICD-10) so everyone knows exactly what was ordered. The app checks if your order is covered (adjudication). And there's a rating system (HEDIS/STAR) to make sure restaurants and apps do a good job.
Cheat Sheet
| Concept | What It Is | Why It Matters |
|---|---|---|
| Payers | Insurance companies, Medicare, Medicaid | They decide what gets paid and how much |
| Providers | Doctors, hospitals, clinics | They deliver care and submit claims |
| Claims Lifecycle | Submit → Adjudicate → Pay/Deny → Appeal | This is how $4.5 trillion moves through the system |
| Coding Systems | CPT (procedures), ICD-10 (diagnoses), DRG (hospital stays) | Universal language for what happened and why |
| Plan Types | HMO, PPO, EPO, POS, HDHP | Determines network rules and cost-sharing |
| Quality Measures | HEDIS scores, CMS STAR ratings | Measures if care is actually good |
The 6 Building Blocks
Payers — Who Pays the Bills?
Payers are the organizations that finance healthcare. When a doctor treats you, the payer gets the bill. There are three main types:
Commercial payers are private insurance companies. The "Big 5" dominate the market:
- UnitedHealth Group — Largest in the US (~50 million members)
- Elevance Health (Anthem) — Blue Cross Blue Shield licensee (~47 million)
- Cigna — Global health services (~17 million)
- Aetna (CVS Health) — Acquired by CVS in 2018 (~23 million)
- Humana — Strong in Medicare Advantage (~17 million)
Government payers cover specific populations:
- Medicare — For people 65+, certain disabled individuals, and end-stage renal disease. Federal program run by CMS.
- Medicaid — For low-income individuals and families. Joint federal-state program (rules vary by state).
- CHIP — Children's Health Insurance Program for kids in families that earn too much for Medicaid but can't afford private insurance.
- VA / TRICARE — For veterans and active military.
Self-insured employers are the hidden giant. About 60% of covered workers are in self-insured plans. The employer bears the financial risk directly, but usually hires an insurance company (like UnitedHealth or Cigna) as a Third-Party Administrator (TPA) to handle claims processing and provider networks.
Providers — Who Delivers Care?
A provider is anyone or any facility that delivers medical care. They come in two flavors:
Facility types:
- Hospitals (inpatient) — You're admitted and stay overnight. Think surgery, ICU, labor and delivery.
- Ambulatory Surgery Centers (ASC) — Same-day surgical procedures. You go home the same day.
- Clinics (outpatient) — Doctor's offices, urgent care, walk-in clinics. Most healthcare happens here.
- Skilled Nursing Facilities (SNF) — Long-term care for patients who need ongoing medical attention.
Provider types:
- Physicians (MD/DO) — Doctors, including primary care and specialists
- Nurse Practitioners (NP) — Advanced practice nurses who can diagnose and prescribe
- Physician Assistants (PA) — Practice medicine under physician supervision
- Specialists — Cardiologists, orthopedists, oncologists, etc.
Every provider gets a National Provider Identifier (NPI) — a unique 10-digit number assigned by CMS. It's like a Social Security Number for healthcare providers. You'll see NPIs on every claim, in every provider directory, and in most healthcare databases.
Claims Lifecycle — How Money Flows
The claims lifecycle is the backbone of healthcare finance. Every time a patient receives care, this process kicks off:
A clean claim rate of 95%+ is the industry target. This means at least 95% of submitted claims should be accepted and processed on the first try without errors.
Coding Systems — The Universal Language
Healthcare uses standardized code sets so that providers, payers, and systems can communicate precisely about what happened during a patient visit. Think of them as the SQL of healthcare — a universal language everyone agrees on.
CPT (Current Procedural Terminology) — 5-digit codes that describe what was done (procedures and services). Maintained by the AMA.
99213— Office visit, established patient, moderate complexity99214— Office visit, established patient, moderate-high complexity27447— Total knee replacement99285— Emergency department visit, high severity
ICD-10-CM (International Classification of Diseases, 10th Revision) — Alphanumeric codes that describe why the patient was seen (diagnoses). Maintained by WHO, adapted by CMS.
E11.9— Type 2 diabetes mellitus without complicationsI10— Essential (primary) hypertensionJ06.9— Acute upper respiratory infection, unspecifiedM54.5— Low back pain
DRG (Diagnosis Related Groups) — Groups inpatient hospital stays by diagnosis for payment purposes. Instead of paying per service, the payer pays a flat rate per DRG.
DRG 470— Major hip/knee joint replacement without complicationsDRG 291— Heart failure and shock with major complications
HCPCS (Healthcare Common Procedure Coding System) — Level II codes for things CPT doesn't cover: medical supplies, ambulance services, durable medical equipment.
A0427— Ambulance service, ALS emergencyE0601— Continuous positive airway pressure (CPAP) device
Plan Types — How Insurance Works
Not all health insurance works the same way. The plan type determines which doctors you can see, whether you need referrals, and how much you pay out of pocket.
| Plan Type | Referrals? | Out-of-Network? | Premiums | Best For |
|---|---|---|---|---|
| HMO | Yes, need PCP referral | No (except emergencies) | Lowest | People who want low costs and don't mind staying in-network |
| PPO | No | Yes (higher cost) | Higher | People who want flexibility to see any doctor |
| EPO | No | No (except emergencies) | Moderate | People who want PPO freedom but in-network only |
| POS | Yes for specialists | Yes (higher cost) | Moderate | Hybrid of HMO and PPO |
| HDHP + HSA | Varies | Varies | Lowest premiums, high deductible | Healthy people who want to save on premiums and use tax-advantaged HSA |
Key cost-sharing terms you'll see in the data:
- Premium — Monthly payment to keep coverage active (whether you use it or not)
- Deductible — Amount you pay out of pocket before insurance kicks in (e.g., $1,500/year)
- Copay — Fixed amount per visit (e.g., $30 for a doctor visit)
- Coinsurance — Your share of costs after deductible, as a percentage (e.g., you pay 20%, insurance pays 80%)
- Out-of-pocket maximum — The most you'll pay in a year. After this, insurance pays 100%.
Quality Measures — Is the Care Good?
Healthcare spending means nothing if patients aren't getting better. Quality measures are how the industry tracks whether care is actually working.
HEDIS (Healthcare Effectiveness Data and Information Set)
- Over 90 measures across preventive care, chronic conditions, access to care, and member satisfaction
- Used by 90% of health plans in the US
- Examples: What percentage of diabetic patients had their A1C tested? How many members got their flu shot? What's the breast cancer screening rate?
- Maintained by NCQA (National Committee for Quality Assurance)
CMS STAR Ratings
- 1 to 5 stars rating system for Medicare Advantage and Part D plans
- Plans rated 4+ stars earn bonus payments from CMS — worth millions of dollars
- Measures include: drug plan customer service, member complaints, member experience, patient safety, managing chronic conditions
- Published annually — directly impacts plan enrollment and revenue
Value-Based Care — The healthcare industry is shifting from fee-for-service (pay per procedure — more procedures = more money) to value-based care (pay for outcomes — healthier patients = more money). This is one of the biggest trends in healthcare data analytics.
Test Yourself
What are the "Big 5" commercial payers?
What's the difference between CPT and ICD-10 codes?
What happens during claims adjudication?
How is an HMO different from a PPO?
What do HEDIS measures evaluate?
Interview Questions
Q: Explain the difference between a denied claim and a rejected claim.
Q: What is the difference between Medicare and Medicaid?
Q: What are HEDIS measures and why do health plans care about them?
Q: What is the difference between fee-for-service and value-based care?
Q: What is a self-insured employer plan and how does it differ from a fully-insured plan?